What Is Managed Care Medicaid?
It refers to how Medicaid benefits are provided to people.
This post was reviewed by our Director of Clinical Excellence and Oversight.
Chances are that if you have Medicaid, you’ve probably heard the term “Managed Care.” If you’re not sure what it means, then it’s time to find out. It’s a pretty important part of your health coverage.
Managed Medicaid simply refers to how Medicaid benefits are provided to people. Here’s a list of everything you need to know about Managed Care plans.

What is Medicaid Managed Care?
Managed Care, sometimes called Managed Medicaid, means that a state has contracted with a private insurance company to provide Medicaid benefits on behalf of the state. The state pays the insurance company a set amount each month, and in return, the company provides their Medicaid members with healthcare services.
What Medical Benefits Does Managed Care Cover?
Managed Care plans cover all of the Medicaid benefits required by the federal government. Some Managed Care plans may also provide extra benefits. Since Managed Care plans are different for each state, benefits may vary. There may also be differences in the health provider networks available.
Can I Get Medical Supplies with My Managed Care Plan?
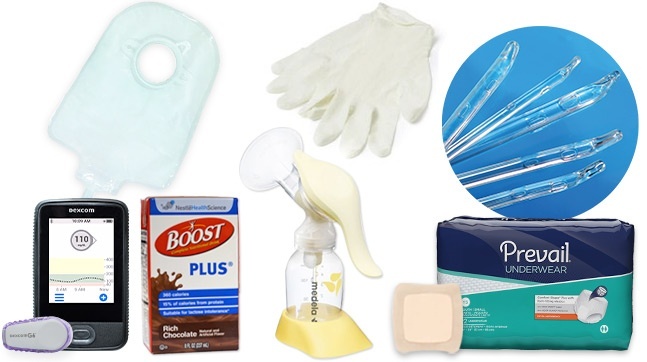
Yes, you can get any medical supplies covered by your Managed Care plan. Here are some of the products you may be eligible to receive:
- Incontinence – Bladder control pads, adult briefs, and more.
- Diabetes – Blood glucose monitors, test strips, and more.
- Wound Care – Gauze, tape, dressings, foam, and more.
- Ostomy – Skin barriers, pouches, wafers, and more.
- Urology – Catheters, lubricant, drainage bags, and more.
- Breast Pumps – Manual and automatic models.
Get Incontinence Supplies Online With Medicaid
No Credit Card | Fast Delivery | 100% Discreet
Does Every State Medicaid Program Have Managed Care Plans?
No, not every state offers Managed Care plans. Some states also use Fee-For Service, which means that the state itself provides healthcare benefits and pays for each individual members’ services directly. To learn more, see What Is Fee-For-Service Medicaid.
To find out if you have a Managed Care Plan or Fee-For-Service, call the number on the back of your insurance card or refer to your plan’s benefit handbook.
Getting Supplies With Managed Care
To get supplies with your insurance, call us today or enroll online for incontinence supplies. Our team of experts will explain which supplies your Medicaid plan covers. We can also set you up with monthly product deliveries if needed, and bill your Medicaid plan for the cost. The process is simple:
- Provide us with some basic information
- We do all the insurance paperwork for you
- Once complete, we’ll ship you monthly product orders and bill your Managed Care plan

It only takes 10 minutes to set up your orders, and it could save you time and money each month on supplies.
Medical Supplies Delivered to Your Door
Accurate Orders | Fast Delivery | Product Expertise