Essential Tips for Traveling When You Have Diabetes
This post was reviewed by our Director of Clinical Excellence and Oversight.

Before You Go
As someone who lives with diabetes, you’re used to planning ahead, which on any given day can mean anything from maintaining your inventory of diabetes management supplies of test strips, lancets, and CGM sensors to anticipating the number of carbs you will eat at each meal. The same thinking applies to travel.
The Centers for Disease Control and Prevention (CDC) recommends visiting your doctor before you travel to make sure you’re fit for the trip. Find out if planned activities could affect your diabetes and, if so, how to prepare. For example, will you be switching time zones? If that’s on your agenda, it’s important to work with your care team to ensure you know how to adjust your insulin when you adjust your time zone.
In addition to information and peace of mind, you’ll want to leave the doctor’s office with two other things:
- a letter stating that you have diabetes and require medical supplies, and
- prescriptions for all your medicines.
Keep these two items in a separate place from the diabetes supplies you are taking with you. That way, if your supplies get lost, you’ll have the information you need to quickly replace them.
Other before-you-go tips:
- Consider purchasing travel insurance in case you require medical care while you’re away.
- Request a diabetic-friendly meal from the airline if food will be served on your flight.
- Identify pharmacies and clinics in the area where you’ll be staying.
- Order a medical ID bracelet and wear it.


Ask your doctor if planned activities might affect your diabetes and, if so, how to prepare. If you’re switching time zones, be sure you know how to adjust your insulin.
Pack with Purpose
Forgetting to pack stuff you need can be annoying. If it’s just a pair of bathing trunks or some shampoo, it’s fairly easy to grab a replacement. When you live with diabetes, however, getting your hands on needed supplies and medications away from home can be a much bigger challenge. Time is often of the essence, because missing a dose of insulin could be dangerous. That’s why it is essential to always have what you need on hand.
The most important packing tip is to bring extras of all diabetes supplies! If you’re traveling for a week, pack two weeks’ worth of oral medications, insulin, and syringes. You’ll also want to have snacks—maybe peanut butter crackers or a nutrition bar—in case your meal is delayed; glucose tablets or gel for low blood sugar; and extra batteries for your glucose meter or insulin pump. Keep your medications in their original bottles and drop them all into a clear plastic zip bag in case anyone questions them.
Your diabetes supplies should always travel with you. If you’re flying, pack them in a carry-on (separate from toiletries) that’s always in your possession. Insulin can be affected by changes in pressure and temperature, so make sure it doesn’t go in your checked bag and is kept at the right temperature! If you’re driving, place supplies inside the car with you, not in an overly hot or cold trunk. Don’t leave your diabetes supplies with the bellman to bring to your room. It can sometimes take hours on a busy day for the bellhops to get everything to the right room and you need to be able to have access to your diabetes supplies at all times.
Will This Fly?
If it’s been a while since you’ve flown, or if you haven’t been on a plane since being diagnosed with diabetes, it’s a good time to review the rules. As we noted above, you can, and should, bring your diabetes supplies on the plane with you as part of your carryon luggage. As you approach the security checkpoint, remove them from your carry-on bag and let the TSA agent know what you’ve got.
Among items permitted through security are Continuous Glucose Monitors; insulin and insulin-loaded vials, jets, and pre-loaded syringes; an unlimited number of unused syringes; lancets, glucose meters, strips, alcohol swabs, and solutions; insulin pumps; and sharps disposal containers.
While the TSA does not require that you have your written prescriptions with you, providing them can speed up the security screening process. Also, when it comes to diabetes supplies, don’t worry about the 3.4-ounce rule that applies to most liquids. The TSA lets you bring medication, glucagon, gels, and other diabetes-related liquids in larger containers.
The TSA offers more information and helpful resources at https://www.tsa.gov/blog/2020/11/13/travel-tip-traveling-diabetes. You can also download a TSA Disability Notification Card at https://www.tsa.gov/sites/default/files/disability_notification_card_508.pdf.

If you’re traveling for a week, bring two weeks’ worth of oral medications, insulin, syringes, and other supplies.
A Few Last Minute Items
Here are some additional tips for traveling safely and smartly with diabetes:
Inject with caution. If you’re planning to inject insulin during your flight, be careful. The pressurized air in the cabin can make it harder to draw up the insulin when using a vial and syringe.

Test more often. With changes in activity, food, and schedules, you should test more often than usual, including before and after meals.

Treat your tootsies. If you will be doing a lot of walking and seeing some great sights, be sure to wear comfortable, well-fitting shoes and socks. Check your feet often, for example, after a flight or a hike.

Move Your body. While you’re in the air, or during a long car ride, point and flex your ankles to keep blood flowing. Try to get up and move around as much as possible. If you are on a plane or a train, even a walk down the aisle to the bathroom will help keep your blood flowing.
Return to travel safely and confidently by having all the insurance, Medicaid, and Medicare-covered medical products you need. Check your supply cabinet, then contact Home Care Delivered to order. And don’t forget to pack for twice the length of time you’ll be gone!
Call 804-885-4101 today and talk with a member of our expert team. Or enter your phone number on the bottom left of the screen and we’ll be glad to reach out. We may not be able to enjoy that upcoming trip with you, but we’ll make sure you have all the supplies you need to travel safely.
There’s no question that traveling with diabetes—like living with diabetes—requires forethought and planning. But once you’re relaxed and are cruising at 35,000 feet, or perhaps cruising an emerald-blue ocean, it will all be worth it!

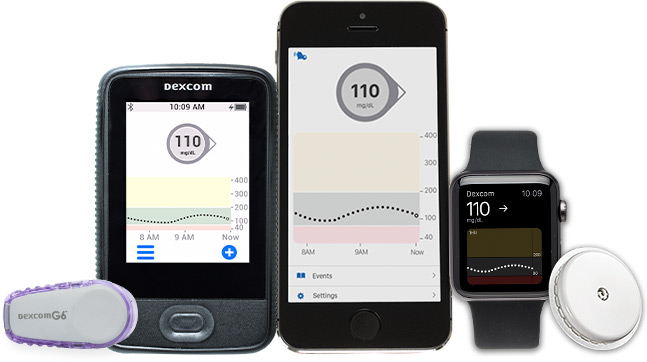
Get Insurance-Covered CGM & Diabetes Supplies
Monthly Deliveries | We Handle the Paperwork
Disclaimer:
Unless otherwise noted, the recommendations in this document were obtained from the sources indicated. Be advised that information contained herein is intended to serve as a useful reference for informational purposes only. HCD cannot be held responsible for the continued accuracy of or for any errors or omissions in the information. All trademarks and registered trademarks are the property of their respective owners.
